A Full Virtual Care Strategy Is More Than Telehealth: Achieve Outcomes, Scale, and ROI with Deviceless Remote Patient Monitoring
October 7, 2020 at 12:48 PM
The COVID-19 pandemic has dramatically accelerated the adoption of telehealth and now remote patient monitoring (RPM) as providers look for new ways to make a clinical impact on population health outside of traditional care settings while also maintaining strong relationships with patients.
The majority of providers have already invested in or are currently evaluating RPM technology to support patients with chronic conditions. As providers continue to identify new applications for these tools and seek to address pressing needs, the market will grow — to a projected $2.1 billion by 2027. But the fundamental challenge of scale is clear: Only by bringing clinically actionable remote monitoring to orders of magnitude can providers achieve the clinical and financial impact they desire.
3 Limitations of Device-Based Remote Patient Monitoring
While the jump from telehealth alone to RPM is a critical step in developing a more comprehensive virtual healthcare strategy, early adopters realize it’s not a straightforward process. Traditional device-based RPM has several significant limitations that prevent it from generating clinical and financial impact:
• Limited accessibility and difficult implementation of devicesPatients who need remote intervention are often older and less tech-savvy. They might struggle to set up Bluetooth or Wi-Fi connections for remote monitoring devices at home. Nurses and doctors will inevitably be asked to help patients troubleshoot the technology.
• High cost and low (or negative) ROI for healthcare organizations
Remote patient monitoring devices perform well for some diseases, but outcomes are only cost effective for a small percentage of patients: those in the highest risk category who can see a significant clinical impact from using expensive devices. However, for other conditions such as behavioral health, social determinants of health (SDoH), and maternal health — device-based monitoring is not necessary or appropriate due to the need to report qualitative data.
• Complex and challenging to operationalize at scale
The pandemic has created a pressing need for remote care in a population much larger than only the high-risk category. Providers need to reach thousands of medium-risk patients with chronic conditions remotely, as frequent in-person appointments have become more challenging. As healthcare organizations identify all eligible candidates who can benefit from remote care, they’re likely to experience difficulty operationalizing care management, handling the logistics of remote monitoring devices, and having enough financial resources to scale the programs.
Shifting From Proof-of-Concept to Scale and Impact:
4 Strengths and Opportunities of Deviceless Remote Patient Monitoring
Provider organizations can collect the same accurate, clinically-actionable data that devices collect — at a fraction of the cost — for considerably more patients using Deviceless RPM.
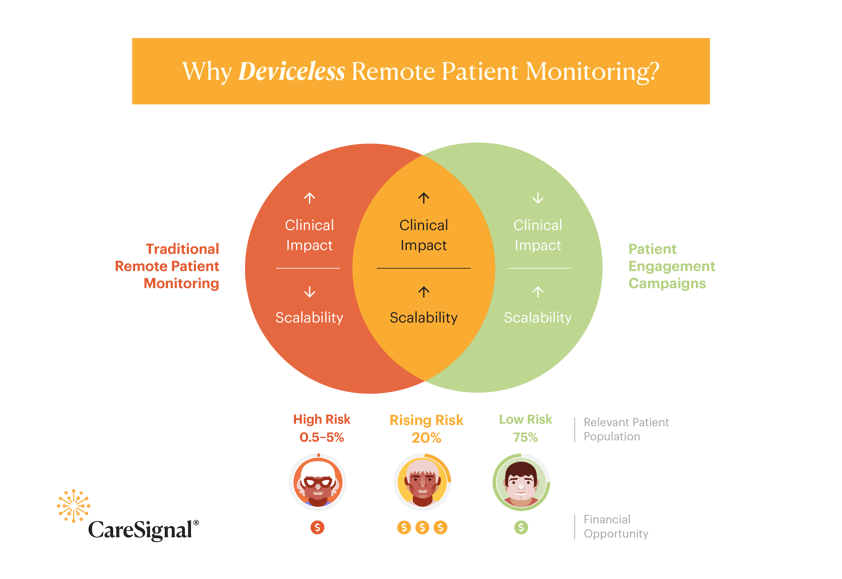
CareSignal’s Deviceless RPM relies on ubiquitous technology — cellphones and text messaging — instead of Bluetooth or Wi-Fi-enabled devices, making it more accessible and much faster to implement. Because patients and providers don’t need additional training to begin using the technology, care managers and RNs can work at the top of their licenses to focus on responsibilities that lead to direct clinical impact rather than being thrust into tech support roles.
• Low cost and positive, rapid ROI for healthcare organizations
CareSignal’s low-cost platform leads to exponentially higher ROI for healthcare organizations. CareSignal can offer Deviceless RPM at a fraction of the cost of device-based alternatives. Greater affordability and accessibility mean its use can expand far beyond the high-risk, chronic condition only category. By increasing touchpoints with these patients remotely, healthcare organizations can lower ED visits and see quick, measurable ROI.
• Scalable to tens of thousands of rising-risk patients, increasing access to care
Because it doesn’t depend on physical devices, CareSignal’s technology is easily scalable to large, disparate populations, such as rising-risk patients with various chronic indications who could greatly benefit from additional, low-touch support. Deviceless RPM collects the same data gathered by traditional RPM devices, allowing providers to reduce ED visits and hospitalizations among much larger patient populations. However, it also gathers more subjective and qualitative metrics, capturing critical context that leads to more actionable information across many more types of conditions.
• Accommodates patients with behavioral health, maternal health, and SDoH
CareSignal Deviceless RPM can be used to monitor depression, substance use disorders, SDoH, maternal health challenges (such as PMAD and breastfeeding adherence), and a range of similar conditions. Patients who use these programs report feeling more comfortable being honest with an automated system versus a human provider, which contributes to highly accurate qualitative data. That information then allows providers to start more productive, empathetic, and timely conversations when they do engage with patients.
Case Studies: Experience Deviceless Remote Patient Monitoring in Action
Healthcare organizations have already realized positive clinical and financial outcomes as they expanded their virtual care strategies with Deviceless RPM.
For example, Esse Health looked to CareSignal to help its Medicare Advantage population with chronic conditions take a more proactive approach to their care. With Deviceless RPM, Esse scaled one care manager’s reach from 100 patients to 1,500, ultimately leading to a 46% reduction in CHF ED visits and a 31% reduction in COPD ED visits. Similarly, Mercy Health System implemented several condition-specific CareSignal programs across patients with chronic conditions and saw a 59% reduction in CHF ED visits and a 30% reduction in COPD ED visits. Review the case studies to learn more.
As more healthcare organizations look beyond telehealth and device-based RPM for technologies and approaches that support sustainable virtual care programs, Deviceless RPM serves as a core component in a comprehensive, scalable virtual health strategy.
Want to learn more about how CareSignal Deviceless RPM can support your organization’s virtual care initiatives? Get in touch with a CareSignal representative and schedule a demo today



